April 24, 2026 | By T. T. Parish, Operational Medical Systems Communications
Team members with the Defense Health Agency’s Operational Medical Systems program management office routinely engage with military medical providers, industry partners, and stakeholders from across the Department of War to refine their product development strategies.
For OPMED’s Warfighter Readiness, Performance, and Brain Health team, end-user touchpoints are designed to collect feedback from clinical and frontline medical providers. They help to mature the development of traumatic brain injury detection capabilities and accelerate the successful completion of the TBI Field Assessment Program, also known as TBI-FAP.
TBI-FAP is unique in the brain health treatment arena, according to Damien Hoffman, a WRPBH product manager whose team is charged with developing and delivering novel TBI medical capabilities to the warfighter. The program, which includes a hemorrhage detection device and a TBI assessment software application, is designed to simplify what has traditionally been a logistically burdensome and overtly subjective process: assessing brain injuries at or near the point of injury.
Over 505,000 traumatic brain injuries have been reported within the Department of War since 2000, ranging from mild to severe, according to Defense Health Agency data. Many TBIs are not accompanied by outwardly presenting symptoms yet can have both short- and long-term health effects. In TBI cases, identifying internal injuries, like intracranial hemorrhage, subdural hematomas, or other non-visible brain damage, is a vital step to ensuring proper triage and treatment across the continuum of care.
“Ultimately, TBI-FAP is uniquely positioned to ensure proper care to casualties, keep warfighters in the fight, and expeditiously return those who have recovered back to duty,” Hoffman said, “and directly aligns with strategic objectives of the Defense Health Agency and the Department of War.”
Field environments demand durable and cost-effective systems, while operational tempo drives the need for those systems to be rapidly deployable, objective, and user-friendly in the hands of frontline medical providers. The TBI field assessment capability is designed to give users the data they need to quickly and confidently make treatment decisions at the speed required by large-scale combat operations.
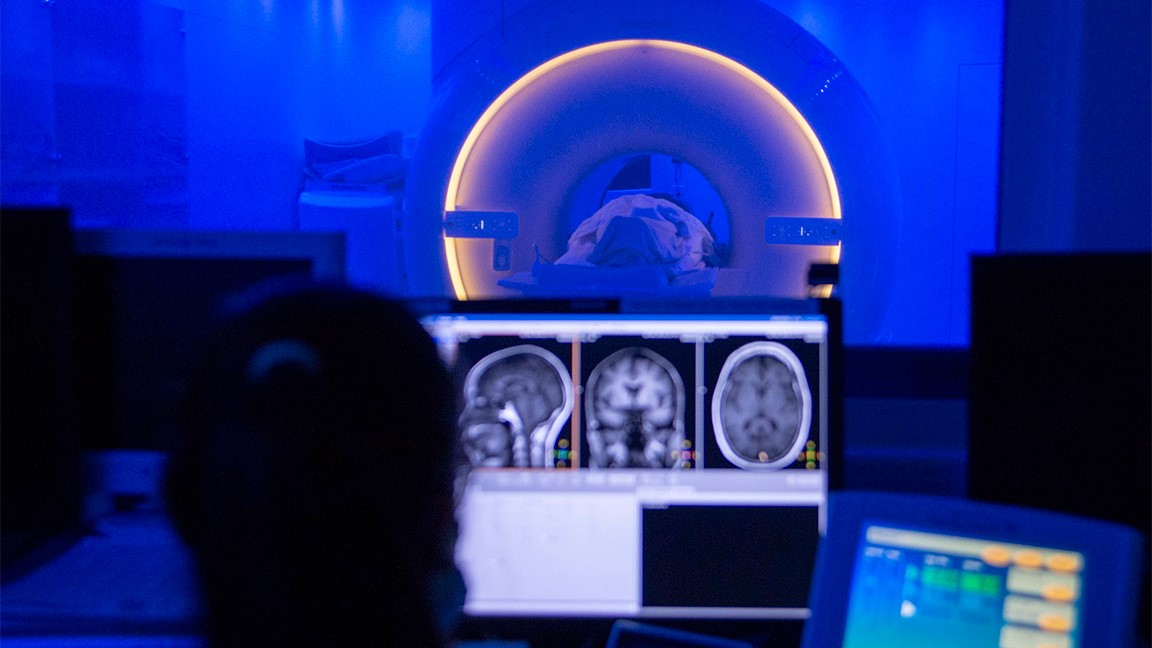
Current options for TBI assessment rely on checklist-based cognitive assessments or robust medical facilities with advanced capabilities like Magnetic Resonance Imaging (MRI) and computed tomography (CT) scans, according to Hoffman. However, while medical imaging is the gold standard for accurate identification of brain traumas, patients typically must be moved from point of injury to access medical imaging—losing precious hours, manpower, and resources without objective information to determine if medevac to higher echelon care is entirely necessary.
The delivered brain hemorrhage detection capability will be portable, lightweight, and field-suitable, and will use non-invasive technologies—such as radiofrequency or near infrared—to assess casualties for intracranial hemorrhage. Accompanying the hemorrhage detection device will be tablet or phone-based applications that offer a suite of digital cognitive assessments. Each of these will be optimized to be easily used by medics, corpsmen, and medical officers, and give accurate, objective data within minutes.
OPMED’s strategic engagements with prospective end users across the service branches also help to ensure the TBI-FAP devices meet the needs of military medical providers and can be integrated with current and emerging medical workflows.
Once fully developed, the fielded technologies—possibly including hardened versions of otherwise commercially available products—will give medics, medical officers, and commanders the information needed to save lives and more efficiently manage constrained or fatigued assets, including evacuation.
Across the joint services, there is significant demand for capabilities like TBI-FAP to fill critical gaps for brain trauma assessment. OPMED’s team, working with military stakeholders, industry partners, and academic experts, is committed to finding the best available solution—and to delivering as soon as possible to our warfighters as the Department of War continues to prepare for conflicts and deter threats across the globe.
“With TBI-FAP, leaders and medical providers alike will have unmatched TBI assessment capabilities, informing frontline treatment decisions with objective information,” said Hoffman. “In turn, this will preserve assets and combat power while ensuring proper TBI care is provided to those who require it.”
About the Operational Medical Systems Program Management Office
The OPMED PMO, part of the Defense Health Agency, is the Department of War’s leading force in medical development and acquisition, focused on enhancing warfighter lethality and readiness. OPMED’s project management teams develop and deliver next-generation, world-class medical capabilities that empower combatant commanders in Large-Scale Combat Operations, particularly within austere environments.